Where there is insurance, there is a scam. Deception can be called a human behavior. Whether it is domestic or British, the annual insurance fraud will bring huge losses to insurance companies, especially in the two common types of insurance and car insurance. In order to circumvent such behavior, insurance companies are trying their best to make money. In Germany, about 2.2 billion euros of claims are unfair each year, and the US Department of Justice’s report claims that fraud has caused the health insurance industry to lose more than $100 billion a year. Although the authenticity of such huge amounts of data is still open to question (some statistics are $3 million to $4 million), the insurance industry does have such a huge hidden gold mine to be tapped today. Long ago, insurers used computers to judge the reasonableness of claims, but the judgment was superficial and the staff needed to review those claims that were marked as “abnormalâ€. According to McKinsey's report, only 10% of all cases marked as "abnormal" are true anomalies. So can we replace artificial labor with artificial intelligence and use deep learning to make reasonable judgments on claims? High accuracy and high efficiency of the rolling stage Employees who review the policy will have some rules in judging whether a claim is true, such as whether the activity is likely to occur, whether the fee is within the specified range, etc. These rules are easy for AI to learn and even better. . After all, human beings often feel sleepy when dealing with such repetitive tasks, and the connection between events is likely to be ignored. For example, if a patient has prescribed many different types of drugs for the same disease but the same effect, then the staff may be in the analysis unit. The irrationality of this behavior is ignored when the price of medicine is reasonable, which is not ignored by artificial intelligence. If you do not consider the negative social effects of unemployment in the insurance company, artificial intelligence crushes human employees in all aspects. The first is efficiency. In the past, there were dozens of employees who spent weeks trying to process claims, only hours in front of artificial intelligence. Second is the accuracy rate. According to the data reported by McKinsey, artificial intelligence can theoretically reduce the current amount of fraudulent protection by about 3%, and each reduction of 1% will bring the benefits of the tens of billions of euros to the insurance industry. The judgment given in this way can reduce the possibility of conflict between the insurance company employee and the policyholder to a certain extent. After all, the presumed result is only a procedure. Image from the McKinsey report The figure above illustrates how artificial intelligence works. The first step is to import all claims into the system, and the AI ​​will initially screen them to filter out all normal cases. In the process, AI is able to identify the association between unusual claims, which helps to strengthen the ability of AI to identify anomalous cases. In the second step, the AI ​​will prioritize the case according to the specific circumstances of the case, and hand the project to the auditor to give reasons for rejecting the claim. How to develop a cognitive system? Although AI can address several important pain points in the regular insurance business, we still need to address the most important data issues in the medical field (here for commercial insurance). Entering the patient's data into the insurance company's information base is a nuisance in itself, but the rapid development of computer vision can speed up data entry. For example, if the medical document identification and analysis cloud platform developed by the doctor is intelligently developed, the invoice and the test list can be identified by scanning, and the digital music library can be entered by itself. After data extraction, the system can preprocess text information through NLP technology. Japanese insurance company Fukoku Mutual Life Insurance has replaced 34 life insurance claims commissioners with IBM Watson since January 2017. Watson can scan the medical records and medical records provided by the hospital, and use NLP technology to refine and process these complex materials, so that employees can free up their hands to deal with other matters related to payment. At the same time, the rich knowledge of artificial intelligence in various fields can also enable insurance companies to reduce their reliance on highly professional employees. With the support of the above technologies, we can simplify the development process of the cognitive system into four parts: 1. Compile and preprocess the appropriate data. Given the sheer volume of data that health insurers have to deal with, this work is trivial, and the key is to ensure data integrity and consistency. At the same time, the test data set should include historical patient data and claim data; 2. Use various statistical models to analyze patient, diagnosis, and claim data. At this stage, it has been possible to determine the correlation between certain diagnoses and the amount claimed. This analysis provides the basis for developing an effective model for marking claims anomalies. The test data is then used to train the cognitive system. Provide additional insurance data and external information through analysis until the final AI begins to learn new data and case patterns independently; 3. For subsequent evaluations and select the system that will ultimately be used, program several cognitive systems and then benchmark against specific metrics. Based on the test results, we choose the system that is the most reliable predictor of the claim; 4. Use the identified system to review new claims cases received under realistic conditions and further improve the algorithm. Which companies are doing this work? Due to the lack of depth in domestic commercial health insurance and the relatively developed commercial insurance system in Europe and the United States, the companies engaged in insurance AI are located abroad. 1. Accolade In 2007, Accolade was founded in Seattle, Washington. Its Maya Intelligence platform helps patients choose the health insurance that best meets their needs based on patient information to reduce healthcare costs. Its partners include both insurance companies and clients with insurance obligations, and currently provide services to more than 1.1 million customers. The company said the platform uses NLP to help analyze and synthesize data in text format and build user context based on factors such as benefit plans, medical history, and claims history to aid in managing patient files. When patients log in, they can access personal data, demographic information, and information about insurance companies. If the user wishes to talk to a nurse or medical assistant about topics such as medical or billing issues, the platform has a referral function that matches the user to the medical professional who best fits his or her background and needs. According to statistics, Accolade successfully reduced health care costs in the second year after working with the Temple University Health System (TUHS), saving a total of $9.8 million. 2, Collective Health Founded in 2013 and headquartered in San Francisco, California, Collective Health integrates demographic data and medical claims to streamline customers' healthcare management processes. In March 2017, Collective Health began a service pilot to provide insurance guidance for employers, employees, and employees' families, and to track their follow-up behavior using the AI ​​system. As of August 2018, Collective Health has 15 employers and 70,000 employees joining the CareX system. 3. Kirontech Founded in 2014 and headquartered in Cambridge, UK, KironMed uses its AI software platform to reduce inefficiencies in the claims management process. KironMed's algorithm uses data from large public databases for training. The algorithm platform synthesizes these data to identify different categories of medical claims and establish patterns related to health insurance fraud (inaccurate billing) or waste (ie, underutilization of services). As of March 2017, the company has raised $3.5 million in Series A financing with venture capital technology company Leap Ventures. 4. Azati Azati was founded in 2001 and is headquartered in Livingston, New Jersey. It uses AI to detect fraud by insurance companies on their customized self-service websites and mobile insurance platforms. When policyholders log on to the platform, they can track and claim through Azat. If the system detects a possible fraud case while analyzing a new claim, a possible case will be sent to the personnel specialist of the insurance company for investigation. The software platform also provides a markup statement that explains why the AI ​​made the judgment. to sum up AI is used in the insurance industry to talk about innovation in a radical sense, and more to integrate a variety of successful AI technologies. But this combination of multiple applications can save huge amounts of insurance for insurance companies around the world. We don't have to worry that advanced analytics will reduce the number of people insured. Only those who want to swindle will stay away from such a system. Normal people will sigh at the unprecedented speed of claims brought by the AI ​​system. Related applications have been slowly developed abroad. On the day when domestic commercial insurance is booming, we may not be worried about choosing insurance.
Anthocyanidin, also known as anthocyanin, is a class of water-soluble natural pigments, flavonoid compounds, widely found in plants. It is also the main coloring substance in plant petals, and most of the colorful colors of fruits, vegetables and flowers are related to it.Anthocyanins belong to the flavonoids (flavonoids) of the phenolic compounds.
Anthocyanins provide a variety of benefits to the human body. Fundamentally, anthocyanins are a powerful anti
There are over 300 different anthocyanins in nature. They come from different fruits and vegetables such as purple sweet potatoes, lingonberries, cranberries, blueberries, black goji berries, grapes, elderberries, blackcurrants, purple carrots, and red kale, ranging in color from red to blue. These anthocyanins mainly contain Delchindin, Cyanidin, Petunidin and Peonidin. Of these, blueberries contain the largest amount of anthocyanins and have the most nutritional value.
Anthocyanins,Cyanidin,Proantho Cyanidins Shaanxi Zhongyi Kangjian Biotechnology Co.,Ltd , https://www.zyplantextract.com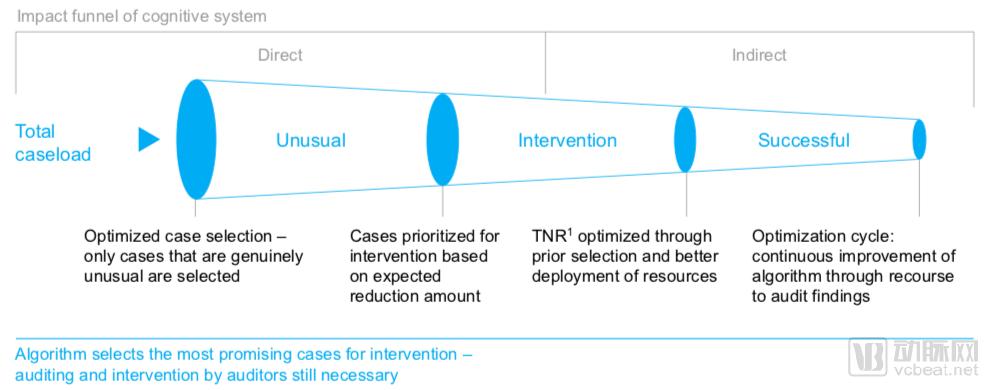
oxidizer, which protects the body from damage caused by a harmful substance called free radicals. Anthocyanins also enhance the elasticity of blood vessels, improve the circulatory system and smoothness of the skin, inhibit inflammation and allergies, and improve the flexibility of joints.
Also used in cosmetics, such as red anthocyanins for lipstick. These commercial pigments (in addition to grape skin pigment) is a common feature of light, heat, oxygen stability, microbial stability. Generally soluble in water and ethanol, insoluble in vegetable oil.